7 Female Reproductive System
WTCS Learning Objectives
- Apply the rules of medical language to build, analyze, spell, pronounce, abbreviate, and define terms as they relate to the female reproductive system
- Identify meanings of key word components of the female reproductive system
- Categorize diagnostic, therapeutic, procedural or anatomic terms related to the female reproductive system
- Use terms related to the female reproductive system
- Use terms related to the diseases and disorders of the female reproductive system
Female Reproductive System Word Parts
Introduction to the Female Reproductive System
The female reproductive system produces gametes and reproductive hormones. In addition, the female reproductive system supports the developing fetus and delivers it to the outside world. The female reproductive system is located primarily inside the pelvic cavity. The female gonads are called ovaries and the gamete they produce is called an oocyte.
Watch this video:
Media 7.1. Reproductive System, Part 1 – Female Reproductive System: Crash Course A&P #40 [Online video]. Copyright 2015 by CrashCourse.
Female Reproductive System Medical Terms
Anatomy (Structures) of the Female Reproductive System
External Female Genitals
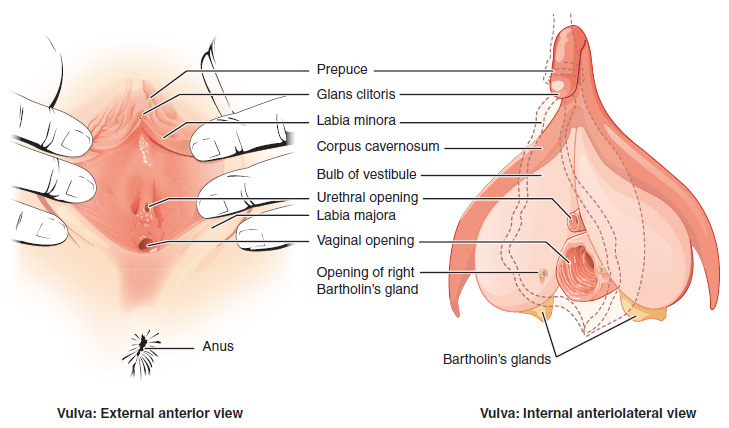
The external female reproductive structures are referred to collectively as the vulva and they include:
- The mons pubis is a pad of fat that is located at the anterior, over the pubic bone. After puberty, it becomes covered in pubic hair.
- The labia majora (labia = “lips”; majora = “larger”) are folds of hair-covered skin that begin just posterior to the mons pubis.
- The labia minora (labia = “lips”; minora = “smaller”) is thinner and more pigmented and extends medially to the labia majora.
- Although they naturally vary in shape and size from woman to woman, the labia minora serve to protect the female urethra and the entrance to the female reproductive tract.
- The superior, anterior portions of the labia minora come together to encircle the clitoris (or glans clitoris), an organ that originates from the same cells as the glans penis and has abundant nerves that make it important in sexual sensation and orgasm. The hymen is a thin membrane that sometimes partially covers the entrance to the vagina.
- The vaginal opening is located between the opening of the urethra and the anus. It is flanked by outlets to the Bartholin’s glands.
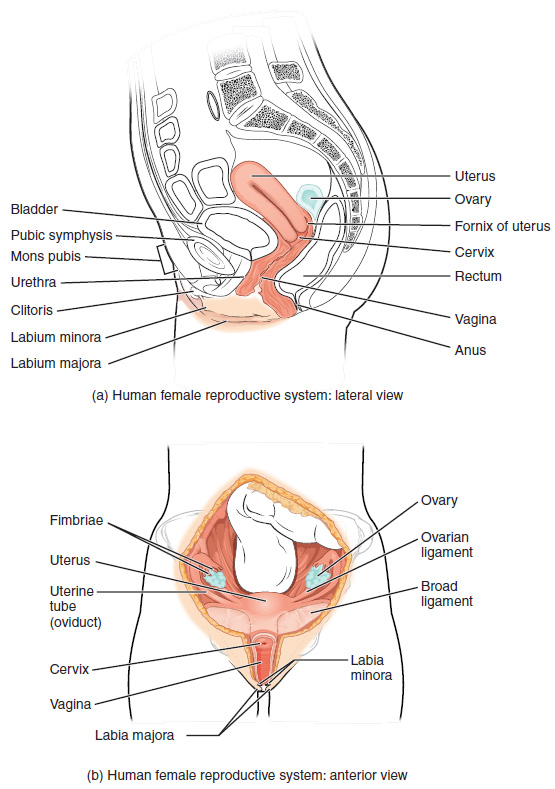
Internal Female Reproductive Organs
Vagina
The vagina is a muscular canal (approximately 10 cm long) that is the entrance to the reproductive tract. It also serves as the exit from the uterus during menses and childbirth. The cervix is the opening to the uterus.
Together, the middle and inner layers allow the expansion of the vagina to accommodate intercourse and childbirth. The thin, perforated hymen can partially surround the opening to the vaginal orifice. The Bartholin’s glands and the lesser vestibular glands (located near the clitoris) secrete mucus, which keeps the vestibular area moist.
The vagina has a normal population of microorganisms that help to protect against infection. There is both pathogenic bacteria, and yeast in the vagina. In a healthy woman, the most predominant type of vaginal bacteria is from the genus Lactobacillus, which secretes lactic acid. the lactic acid protects the vagina by maintaining an acidic pH (below 4.5).
Lactic acid, in combination with other vaginal secretions, makes the vagina a self-cleansing organ. However, douching can disrupt the normal balance of healthy microorganisms, and increase a woman’s risk for infections and irritation. It is recommend that women do not douche and that they allow the vagina to maintain its normal healthy population of protective microbial flora.
Ovaries
The ovaries are the female gonads. There are two, one at each entrance to the fallopian tube. They are each about 2 to 3 cm in length, about the size of an almond. The ovaries are located within the pelvic cavity. The ovary itself is attached to the uterus via the ovarian ligament. This grouping of an oocyte and its supporting cells is called a follicle.
The Fallopian Tubes
The fallopian tubes are the conduit of the oocyte from the ovary to the uterus. Each of the two fallopian tubes is close to, but not directly connected to, the ovary. Instead fimbriae catch the oocyte like a baseball in a glove. The middle region of the tube, called the ampulla, is where fertilization often occurs.
The uterus is the muscular organ that nourishes and supports the growing embryo. Its average size is approximately 5 cm wide by 7 cm long and it has three sections.
- The portion of the uterus superior to (pertaining to above) the opening of the uterine tubes is called the fundus.
- The middle section of the uterus is called the body of uterus (or corpus).
- The cervix is the narrow inferior portion of the uterus that projects into the vagina.
- The cervix produces mucus secretions that become thin and stringy under the influence of high systemic plasma estrogen concentrations, and these secretions can facilitate sperm movement through the reproductive tract.
The wall of the uterus is made up of three layers:
- Perimetrium: the most superficial layer and serous membrane.
- Myometrium: a thick layer of smooth muscle responsible for uterine contractions.
- Endometrium: the innermost layer containing a connective tissue lining covered by epithelial tissue that lines the lumen. It provides the site of implantation for a fertilized egg, and sheds during menstruation if no egg is fertilized.
Concept Check
- Write or draw out the components of the pathway that an oocyte takes from beginning to end.
Physiology (Function) of the Female Reproductive System-Ovulation
Following ovulation, the Fallopian tube receives the oocyte. Oocytes lack flagella, and therefore cannot move on their own.
- High concentrations of estrogen that occur around the time of ovulation induce contractions of the smooth muscle along the length of the Fallopian tube.
- These contractions occur every 4 to 8 seconds, causing the oocyte to flow towards the uterus, through the coordinated beating of the cilia that line the outside and lumen of the length of the Fallopian tube which pulls the oocyte into the interior of the tube.
- Once inside, the muscular contractions and beating cilia move the oocyte slowly toward the uterus.
- When fertilization does occur, sperm typically meet the egg while it is still moving through the ampulla.
Watch this video:
Watch this video on ovulation from MedLine Plus to observe ovulation and its initiation in response to the release of FSH and LH from the pituitary gland.
Media 7.2. Ovulation. From Betts, et al., 2021. Licensed under CC BY 4.0.
The three phases of the menstrual cycle are:
- The menses phase of the menstrual cycle is the phase during which reproductive hormone levels are low, the woman menstruates, and the lining is shed. The menses phase lasts between 2 – 7 days with an average of 5 days.
- The proliferative phase is when menstrual flow ceases and the endometrium begins to proliferate . During this phase reproductive hormones are working in homeostasis to trigger ovulation on approximately day 14 of a typical 28-day menstrual cycle. Ovulation marks the end of the proliferative phase.
- The secretory phase the endometrial lining prepares for implantation of a fertilized egg. If no pregnancy occurs within approximately 10- 12 days the endometrium will grow thinner and shed starting the first day of the next cycle.
Anatomy Labeling Activity
Female Reproductive System Terms not Easily Broken into Word Parts
Female Reproductive System Medical Abbreviations
Diseases and Disorders of the Female Reproductive System
Cancer
Breast Cancer
Breast cancer starts in the cells that line the ducts or the lobule of the breast. Some warning signs include a new lump in the breast or axilla, thickening or swelling, irritation or dimpling of the breast skin, redness or flaky skin, pain, discharge, all in the breast or nipple area, and change in breast size. Risk factors include family history, obesity, hormonal treatment and changes in breast cancer-related genes (BRCA1 or BRCA2) (Centers for Disease Control and Prevention, n.d.; Cancer Care Ontario, n.d.).
Treatment options include chemotherapy, radiation and surgical interventions such as mastectomy, biopsy, incision and drainage and mammoplasty (Cancer Treatment Centers of America, n.d.). To learn more about breast cancer, view the Cancer Treatment Centers of America webpage.
Cervical Cancer
Cervical cancer is typically slow-growing cancer and is highly curable when found and treated early. Advanced cervical cancer may cause abnormal bleeding or discharge from the vagina such as bleeding after sex. It is diagnosed during a Papanicolaou test (or Pap smear) which looks for precancers, cell changes, on the cervix. The Pap test can find cervical cancer early, when treatment is most effective. The Pap test only screens for cervical cancer (Centers for Disease Control and Prevention, 2019).
The HPV (Human papillomavirus) test looks for HPV strains which is the virus that can cause precancerous cell changes. Almost all cervical cancers are caused by HPV. HPV is a common virus that is passed from one person to another during sexual contact. In Canada, there is the HPV vaccine. The age of administration varies between states. To learn more about cervical cancer please visit the Centers for Disease Control and Prevention’s cervical cancer factsheet (PDF file).
Endometriosis
Endometriosis is an abnormal condition of the endometrium. Endometriosis occurs when this tissue grows and implants outside the uterus. The female hormone estrogen causes these implants to grow, bleed, and break down. They are implanted outside the uterus have no way to leave the body. They become painful, inflamed, and swollen. The inflammation causes scar tissue around nearby organs which can interfere with their normal functioning and cause pain (Mayo Clinic, 2019).
Endometriosis generally appears between the ages of 15 and 50. Signs and symptoms may include dysmenorrhea, lumbago, dyspareunia, menstrual irregularity and infertility. One-third of women diagnosed with endometriosis have no symptoms at all. Diagnosis may include laparoscopy and endometrial biopsy. Treatment may include medication, surgical interventions such as hysterectomy and oophorectomy. The cause of endometriosis is unknown (Mayo Clinic, 2019). To learn more about endometriosis visit the Mayo Clinic’s Endometriosis profile.
PCOS
Polycystic Ovary Syndrome (PCOS) has no known etiology but researchers have linked it to excessive insulin production. Excessive insulin in the body can release extra male hormones in women. Since the ovaries produce high levels of androgens this causes the eggs to develop into cysts and instead of releasing during ovulation, the cysts build up and enlarge. The most common symptoms of PCOS include oligomenorrhea, amenorrhea, polymenorrhea, enlarged ovaries with multiple small painless cysts or follicles that form in the ovary, acrochordons, acanthosis nigricans, hirsuitism, thinning hair, acne, weight gain, anxiety, depression, hyperglycemia, and infertility (Mayo Clinic, 2020).
Treatments like medications such as birth control pills or antiandrogens can help balance the hormones in your body and relieve some of the symptoms (Mayo Clinic, 2020). To learn more about Polycystic Ovary Syndrome visit the Mayo Clinic’s PCOS profile.
Sexually Transmitted Infections (STIs)
The terms for Sexually Transmitted Infections (STI) and Sexuality Transmitted Diseases (STD) are often used interchangeably. Sexuality Transmitted Diseases (STD) implies the disease was acquired through sexual transmission. A disease is a disorder of structure or function in a human, which produces specific signs or symptoms. A disease must be managed, as with the case of Human Immunodeficiency Virus (which can also be acquired to through the transmission of other bodily fluids; thus not solely sexual transmission). The treatment may include antiretrovirals or anti-virals (Urology Care Foundation, 2019).
Chlamydia (CT)
Chlamydia is one of the most common sexually transmitted infections (STIs) caused by bacteria that infect the cervix, urethra and other reproductive organs. Chlamydia is easy to treat and can be cured. Many people with chlamydia do not have any symptoms and unknowingly pass the infection to their sexual partner(s). If symptoms develop, they usually appear two to six weeks after sexual contact with an infected person. While females are most often asymptomatic they may experience cervicitis. Left untreated, chlamydia in females can lead to Pelvic Inflammatory Disease (PID) which can cause permanent damage to the reproductive organs and subsequent infertility (Centers for Disease Control and Prevention, 2021a).
Chlamydia spreads through unprotected oral, anal or vaginal sex with an infected person. Chlamydia can be spread to the eyes via the hands with direct contact of infected fluids. Until a patient finishes their treatment, they continue to have the infection and can continue to pass it to others. Chlamydia is treated with antibiotic pills. If the patient has epididymitis, they may need to be hospitalized and be treated with intravenous (IV) antibiotics. All sexual partners within the past 60 days should be examined, treated, and informed that having no symptoms does not mean there is no infection (Centers for Disease Control and Prevention, 2021a).
Gonorrhea (Gonococcus) – (GC)
Gonorrhea is a sexually transmitted infection (STI) caused by bacteria that infects the cervix, urethra and other reproductive organs. Infections can also infect the throat and anus. Gonorrhea can be treated and cured. Many people infected with Gonorrhea have no symptoms and can unknowingly pass the infection on to their sexual partner(s). If symptoms develop, they may appear two to seven days after sexual contact with an infected person. Symptoms vary depending on which part of the body is infected. Females may experience abnormal vaginal bleeding, discharge, or dysuria. Left untreated, Gonorrhea in females may lead to pelvic inflammatory disease and fertility complications such as ectopic pregnancy. Gonorrhea infection from oral sex may lead to sore throat and swollen glands. Gonorrhea infection from anal sex may cause itchiness and discharge from the anus. Gonorrhea is spread through unprotected oral, vaginal or anal sex with an infected person. Until the patient finishes their treatment, they continue to have the infection and can pass it to others (Centers for Disease Control and Prevention, 2021b).
Gonorrhea is treated with oral antibiotics in combination with an intramuscular (IM) injection. It is important that one completes the treatment and abstain from unprotected sexual activity for at least seven days following treatment. All sexual partners within the past 60 days should be examined, treated and informed that having no symptoms does not mean there is no infection (Centers for Disease Control and Prevention, 2021b).
Reportable Diseases
Both chlamydia and gonorrhea are reportable diseases and the provider should report cases to local and state public health agencies as well as to the Centers for Disease Control and Prevention. Requirements and procedures vary by county and state. For more information see Medline’s Reportable Diseases list.
Human Papillomavirus- HPV
HPV is a common sexually transmitted infection (STI). Both males and females can be infected with HPV. Almost three quarters of sexually active individuals have been exposed to HPV during their lifetime. There are over 100 strains of HPV and some strains of HPV can cause visible genital warts. The warts are usually painless but may be itchy, uncomfortable and hard to treat. Some strains of HPV cause genital, anal, throat and cervical cancers. HPV spreads through sexual activity and skin-to-skin contact in the genital area with an infected person. Since some people are asymptomatic they don’t know they have the virus and consequently pass the virus to their sexual partners. Treatments are available for genital warts but there is no cure for HPV (Centers for Disease Control and Prevention, 2021c). To learn more about HPV symptoms, treatments, and prognosis visit the CDC HPV Fact Sheet.
HPV Vaccine
A vaccine is available for 9 HPV strains. This vaccine, often known by the brand name Gardasil® 9, assists the immune system in protecting the body against infections and diseases caused by HPV (National Cancer Institute, 2019). To learn more about HPV vaccines, please visit the National Cancer Institute’s HPV Vaccine Fact Sheet.
Herpes Simplex Virus (HSV)
Genital herpes is a sexually transmitted infection (STI) that is caused by a virus called herpes simplex virus (HSV). There are two types of herpes simplex viruses:
- Type 1- oral herpes or cold sores (HSV-1)
- Type 2- genital herpes (HSV-2).
These viruses are very similar and either type can cause genital herpes or cold sores. Symptoms might include dysuria, enlarged glands, myalgia, arthralgia and fever. Once a patient is infected with HSV, the virus remains in their body even after the symptoms are gone and can cause recurring outbreaks. Between the outbreaks, the virus stays in their body. When the virus becomes active again, the symptoms return but are usually less painful and heal faster. Recurring outbreaks vary from person-to-person, however they can be triggered by emotional or physical stress, exposure to sunlight, hormonal changes, poor nutrition, sexual intercourse, lack of sleep or a low immune system (Centers for Disease Control and Prevention, 2021d).
Herpes is spread through direct contact with the sores or blisters of an infected person. Contact (and transfer of the virus) can occur from genitals-to-genitals, mouth-to-genitals or mouth-to-mouth. Herpes can also be passed to the anal area. Herpes spreads easily during sexual contact while symptoms are present, or just before an outbreak of symptoms. An infected person may spread herpes even when they have no symptoms; this is called asymptomatic shedding. One can spread the herpes virus to other parts of their body after touching the sores; autoinoculation. The fingers, eyes and other body areas can accidentally become infected in this way. Hand washing after touching sores and blisters is recommended to prevent spreading the virus (Centers for Disease Control and Prevention, 2021d).
There is no cure for herpes. Antiviral pills help to reduce symptoms and speed the healing of blisters or sores and are prescribed by a doctor. Treatment of symptoms may be managed with medication for pain, bath salts, cold compresses and urinating in water may help to relieve discomfort. Keep the infected area clean and dry, wear cotton underwear and loose clothing to reduce discomfort. All sexual partner(s) should be informed. The only way to reduce the risk of transmission of herpes is to avoid direct contact with the sores and to use condoms. Condoms will reduce but not eliminate risk as the virus can be present and shed from the skin in the genital area (Centers for Disease Control and Prevention, 2021d).
To learn more about the symptoms, complications, treatments and prognosis of HSV please see the CDC Herpes Fact Sheet.
Female Reproductive System Medical Abbreviations
Medical Terms in Context
Medical Specialties and Procedures related to the Female Reproductive System
Gynecology
A gynecologist is a specialist in the area of gynecology focusing on the diagnosis, treatment, management and prevention of diseases and disorders of the female reproductive system. Obstetrics is a specialty that provides care through pregnancy, labour, and puerperium. Further subspecialties in women’s health include contraception, reproductive endocrinology, infertility, adolescent gynecology, endoscopy and gynecological oncology (American Board of Medical Specialties, n.d.). To learn more about obstetrics or gynecology please visit the specialty and subspecialty page of the American Board of Obstetrics and Gynecology.
Hysterectomy
A hysterectomy is done to stage or treat female reproductive cancers, treat precancerous conditions of the cervix and some non-cancerous conditions that have not responded to other forms of treatment. There are three types of hysterectomy:
- A total hysterectomy removes both the uterus and the cervix.
- A subtotal hysterectomy removes the uterus only.
- A radical hysterectomy removes uterus, cervix, part of the vagina, and ligaments.
Sometimes the ovaries and fallopian tubes are removed at the same time that a hysterectomy is done. A bilateral salpingo-oophorectomy (BSO) removes both ovaries and fallopian tubes. A unilateral salpingo-oophorectomy removes one ovary and one Fallopian tube (National Women’s Health Network, 2015). To learn more about hysterectomy please follow visit the National Women’s Health Network’s page on hysterectomies.
Test Yourself
References
American Board of Medical Specialties. (n.d.). American Board of Obstetrics and Gynecology Specialties & Subspecialties. https://www.abms.org/board/american-board-of-obstetrics-gynecology/
Cancer Treatment Centers of America. (n.d.) Breast Cancer. https://www.cancercenter.com/cancer-types/breast-cancer
Centers for Disease Control and Prevention. (n.d.). Breast cancer: What you need to know. CDC: Cancer. https://www.cdc.gov/cancer/breast/pdf/breastcancerfactsheet.pdf
Centers for Disease Control and Prevention. (2019, January). Cervical cancer: Inside knowledge about gynecolocic cancer. CDC: Cancer. https://www.cdc.gov/cancer/cervical/pdf/cervical_facts.pdf?src=SocialMediaToolkits
Centers for Disease Control and Prevention. (2021a). Chlamydia – CDC Fact Sheet (Detailed). https://www.cdc.gov/std/chlamydia/stdfact-chlamydia-detailed.htm
Centers for Disease Control and Prevention. (2021b). Gonorrhea – CDC Fact Sheet (Detailed). https://www.cdc.gov/std/gonorrhea/stdfact-gonorrhea-detailed.htm
Centers for Disease Control and Prevention. (2021c). HPV Infection – Fact Sheet. https://www.cdc.gov/std/hpv/stdfact-hpv.htm
Centers for Disease Control and Prevention. (2021d). Genital Herpes – CDC Fact Sheet (Detailed). https://www.cdc.gov/std/herpes/stdfact-herpes-detailed.htm
[CrashCourse]. (2015, October 2015). Reproductive system, part 1 – female reproductive system: Crash course A&P #40 [Video]. YouTube. https://www.youtube.com/watch?v=RFDatCchpus
Mayo Clinic. (2019). Endometriosis profile. https://www.mayoclinic.org/diseases-conditions/endometriosis/symptoms-causes/syc-20354656
Mayo Clinic. (2020). Polycystic ovarian syndrome profile. https://www.mayoclinic.org/diseases-conditions/pcos/symptoms-causes/syc-20353439
MedlinePlus. (2021, April). Reportable Diseases. https://medlineplus.gov/ency/article/001929.htm
National Cancer Institute. (2019, January). Human Papillomavirus (HPV) Vaccines. https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv-vaccine-fact-sheet
National Women’s Health Network. (2015). Hysterectomy in the United States. https://nwhn.org/hysterectomy/
Urology Care Foundation. (2019). What are sexually transmitted infections (STIs) or diseases (STDs). Urology Care Foundation: Urologic Conditions. https://www.urologyhealth.org/urologic-conditions/sexually-transmitted-infections#Acquired_Immune_Deficiency_Syndrome_(AIDS)
Unless otherwise indicated, this chapter contains material adapted from Anatomy and Physiology (on OpenStax), by Betts, et al. and is used under a a CC BY 4.0 international license. Download and access this book for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction.
haploid reproductive cells that contribute genetic material to form an offspring
A female reproductive organ in which ova or eggs are produced.
A female gamete
Also known as greater vestibular glands they are responsible to secrete mucus to keep the vestibular area moist
washing the vagina with fluid
reproduce rapidly
biological process that results in stable equilibrium
armpit
Excision of breast(s) and or breast tissue
surgical repair of the breast particularly after a mastectomy
The innermost layer containing a connective tissue lining covered by epithelial tissue that lines the lumen.Provides the site of implantation for a fertilized egg
Sheds during menstruation if no egg is fertilized.
painful periods
lower back pain
painful intercourse
process of viewing internal organs in the abdomen
Surgical removal of the uterus
surgical removal of the fallopian/uterine tubes
Hormones that affect growth and reproduction. Typically referred to as "male hormones," however the female body produces small amounts of androgens as well.
Infrequent or irregular periods
absence of periods
excessive bleeding during one's period
skin tags, teardrop-sized pieces of skin that can be as large as raisins and are typically found in the armpits or neck area
disorder that causes darkening and thickening of the skin on the neck, groin, underarms, or skin folds
excess hair all over the body
a group of medications that counteract the effects of male hormones.
treatment that works against the virus replication
treatments that work effectively against a virus.
Inflammation of the cervix
swelling/inflammation of the epididymis
painful urination
Antiobiotics are medications that stop bacterial infections.
pertaining to within the muscle
pertaining to without symptoms
pain in the muscles
painful joint(s)
self inoculation
Specialist in the study and treatment of the female reproductive system
The study of the female reproductive system
Time directly after childbirth
The study of endocrine glands and hormones
Process of viewing internally
pertaining to both sides
pertaining to one side

