Nursing Process
4.6 Planning
Open Resources for Nursing (Open RN)
Planning is the fourth step of the nursing process (and the fourth Standard of Practice set by the American Nurses Association). This standard is defined as, “The registered nurse develops a collaborative plan encompassing strategies to achieve expected outcomes.” The RN develops an individualized, holistic, evidence-based plan in partnership with the health care consumer, family, significant others, and interprofessional team. Elements of the plan are prioritized. The plan is modified according to the ongoing assessment of the health care consumer’s response and other indicators. The plan is documented using standardized language or terminology.[1]
After expected outcomes are identified, the nurse begins planning nursing interventions to implement. Nursing interventions are evidence-based actions that the nurse performs to achieve patient outcomes. Just as a provider makes medical diagnoses and writes prescriptions to improve the patient’s medical condition, a nurse formulates nursing diagnoses and plans nursing interventions to resolve patient problems. Nursing interventions should focus on eliminating or reducing the related factors (etiology) of the nursing diagnoses when possible.[2] Nursing interventions, goals, and expected outcomes are written in the nursing care plan for continuity of care across shifts, nurses, and health professionals.
Planning Nursing Interventions
You might be asking yourself, “How do I know what evidence-based nursing interventions to include in the nursing care plan?” There are several sources that nurses and nursing students can use to select nursing interventions. Many agencies have care planning tools and references included in the electronic health record that are easily documented in the patient chart. Nurses can also refer to other care planning books our sources such as the Nursing Interventions Classification (NIC) system. Based on research and input from the nursing profession, NIC categorizes and describes nursing interventions that are constantly evaluated and updated. Interventions included in NIC are considered evidence-based nursing practices. The nurse is responsible for using clinical judgment to make decisions about which interventions are best suited to meet an individualized patient’s needs.[3]
Direct and Indirect Care
Nursing interventions are considered direct care or indirect care. Direct care refers to interventions that are carried out by having personal contact with patients. Examples of direct care interventions are wound care, repositioning, and ambulation. Indirect care interventions are performed when the nurse provides assistance in a setting other than with the patient. Examples of indirect care interventions are attending care conferences, documenting, and communicating about patient care with other providers.
Classification of Nursing Interventions
There are three types of nursing interventions: independent, dependent, and collaborative. (See Figure 4.12[4] for an image of a nurse collaborating with the health care team when planning interventions.)

Independent Nursing Interventions
Any intervention that the nurse can independently provide without obtaining a prescription is considered an independent nursing intervention. An example of an independent nursing intervention is when the nurses monitor the patient’s 24-hour intake/output record for trends because of a risk for imbalanced fluid volume. Another example of independent nursing interventions is the therapeutic communication that a nurse uses to assist patients to cope with a new medical diagnosis.
Example. Refer to Scenario C in the “Assessment” section of this chapter. Ms. J. was diagnosed with Fluid Volume Excess. An example of an evidence-based independent nursing intervention is, “The nurse will reposition the patient with dependent edema frequently, as appropriate.”[5] The nurse would individualize this evidence-based intervention to the patient and agency policy by stating, “The nurse will reposition the patient every 2 hours.”
Dependent Nursing Interventions
Dependent nursing interventions require a prescription before they can be performed. Prescriptions are orders, interventions, remedies, or treatments ordered or directed by an authorized primary health care provider.[6] A primary health care provider is a member of the health care team (usually a physician, advanced practice nurse, or physician’s assistant) who is licensed and authorized to formulate prescriptions on behalf of the client. For example, administering medication is a dependent nursing intervention. The nurse incorporates dependent interventions into the patient’s overall care plan by associating each intervention with the appropriate nursing diagnosis.
Example. Refer to Scenario C in the “Assessment” section of this chapter. Ms. J. was diagnosed with Fluid Volume Excess. An example of a dependent nursing intervention is, “The nurse will administer scheduled diuretics as prescribed.”
Collaborative Nursing Interventions
Collaborative nursing interventions are actions that the nurse carries out in collaboration with other health team members, such as physicians, social workers, respiratory therapists, physical therapists, and occupational therapists. These actions are developed in consultation with other health care professionals and incorporate their professional viewpoint.[7]
Example. Refer to Scenario C in the “Assessment” section of this chapter. Ms. J. was diagnosed with Fluid Volume Excess. An example of a collaborative nursing intervention is consulting with a respiratory therapist when the patient has deteriorating oxygen saturation levels. The respiratory therapist plans oxygen therapy and obtains a prescription from the provider. The nurse would document “The nurse will manage oxygen therapy in collaboration with the respiratory therapist” in the care plan.
Individualization of Interventions
It is vital for the planned interventions to be individualized to the patient to be successful. For example, adding prune juice to the breakfast meal of a patient with constipation will only work if the patient likes to drink the prune juice. If the patient does not like prune juice, then this intervention should not be included in the care plan. Collaboration with the patient, family members, significant others, and the interprofessional team is essential for selecting effective interventions. The number of interventions included in a nursing care plan is not a hard and fast rule, but enough quality, individualized interventions should be planned to meet the identified outcomes for that patient.
Creating Nursing Care Plans
Nursing care plans are created by registered nurses (RNs). Documentation of individualized nursing care plans are legally required in long-term care facilities by the Centers for Medicare and Medicaid Services (CMS) and in hospitals by The Joint Commission. CMS guidelines state, “Residents and their representative(s) must be afforded the opportunity to participate in their care planning process and to be included in decisions and changes in care, treatment, and/or interventions. This applies both to initial decisions about care and treatment, as well as the refusal of care or treatment. Facility staff must support and encourage participation in the care planning process. This may include ensuring that residents, families, or representatives understand the comprehensive care planning process, holding care planning meetings at the time of day when a resident is functioning best and patient representatives can be present, providing sufficient notice in advance of the meeting, scheduling these meetings to accommodate a resident’s representative (such as conducting the meeting in-person, via a conference call, or video conferencing), and planning enough time for information exchange and decision-making. A resident has the right to select or refuse specific treatment options before the care plan is instituted.”[8] The Joint Commission conceptualizes the care planning process as the structuring framework for coordinating communication that will result in safe and effective care.[9]
Many facilities have established standardized nursing care plans with lists of possible interventions that can be customized for each specific patient. Other facilities require the nurse to develop each care plan independently. Whatever the format, nursing care plans should be individualized to meet the specific and unique needs of each patient. See Figure 4.13[10] for an image of a standardized care plan.
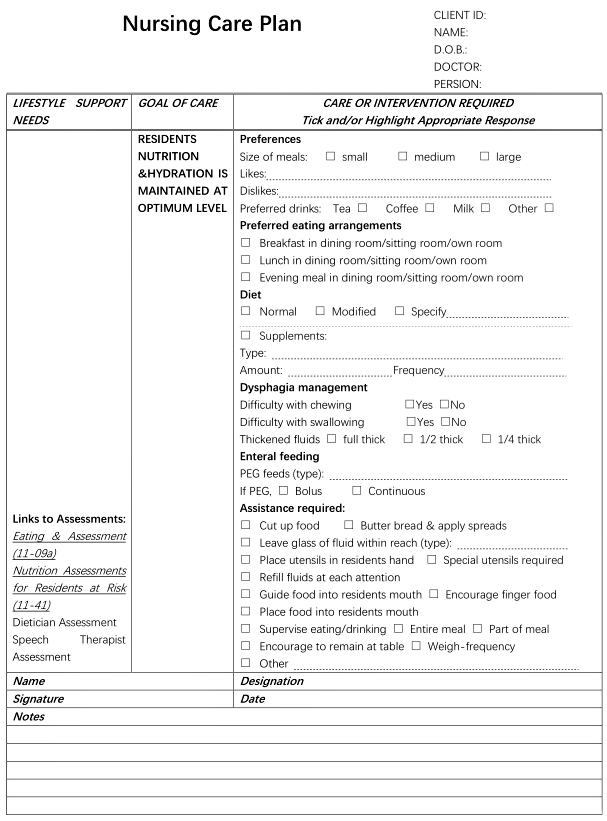
Nursing care plans created in nursing school can also be in various formats such as concept maps or tables. Some are fun and creative, while others are more formal. Appendix B contains a template that can be used for creating nursing care plans.
- American Nurses Association. (2021). Nursing: Scope and standards of practice (4th ed.). American Nurses Association. ↵
- Herdman, T. H., & Kamitsuru, S. (Eds.). (2018). Nursing diagnoses: Definitions and classification, 2018-2020. Thieme Publishers New York. ↵
- Butcher, H. K., Bulechek, G. M., Dochterman, J. M., & Wagner, C. M. (2018). Nursing interventions classifications (NIC) (7th ed.). Elsevier. ↵
- "400845937-huge.jpg" by Flamingo Images is used under license from Shutterstock.com ↵
- Butcher, H. K., Bulechek, G. M., Dochterman, J. M., & Wagner, C. M. (2018). Nursing interventions classifications (NIC) (7th ed.). Elsevier. ↵
- NCSBN. (n.d.). 2019 NCLEX-RN test plan. https://www.ncsbn.org/2019_RN_TestPlan-English.htm ↵
- Vera, M. (2020). Nursing care plan (NCP): Ultimate guide and database. https://nurseslabs.com/nursing-care-plans/#:~:text=Collaborative%20interventions%20are%20actions%20that,to%20gain%20their%20professional%20viewpoint. ↵
- Centers for Medicare and Medicaid Services. (2017). State operations manual: Appendix PP - Guidance to surveyors for long term care facilities. https://www.cms.gov/Regulations-and-Guidance/Guidance/Manuals/downloads/som107ap_pp_guidelines_ltcf.pdf ↵
- The Joint Commission (n.d.). Standards and guides pertinent to nursing practice. https://www.jointcommission.org/resources/for-nurses/nursing-resources/ ↵
- "Figure 3-3. An example of a nursing care plan in an Australian residential aged care home..png" by NurseRecord is licensed under CC BY-SA 4.0 ↵
Cataracts: Opacity of the lens of the eye that causes clouded, blurred, or dim vision. Cataracts can be removed with surgery that replaces the lens with an artificial lens.
Diabetic retinopathy: A complication of diabetes mellitus due to damaged blood vessels in the retina. If found early, treatments, such as laser treatment that can help shrink blood vessels, injections that can reduce swelling, or surgery, can prevent permanent vision loss.
Glaucoma: Gradual loss of peripheral vision caused by elevated intraocular pressure that leads to progressive damage to the optic nerve.
Kinesthetic impairment: An altered sense of touch that can cause difficulty in performing fine motor tasks.
Macular degeneration: Loss of central vision with symptoms such as blurred central vision, distorted vision that causes difficulty driving and reading, and the requirement for brighter lights and magnification for close-up visual activities.
Perception: The interpretation of sensation during the sensory process.
Presbycusis: Age-related hearing loss.
Presbyopia: The impairment of near vision and accommodation as the lens of the eye gradually becomes thicker and loses flexibility as a person ages.
Proprioception: The sense of the position of our bones, joints, and muscles.
Reaction: The response that individuals have to a perception of a received stimulus.
Reception: The initial part of the sensory process when a nerve cell or sensory receptor is stimulated by a sensation.
Sensory deprivation: A condition that occurs when there is a lack of sensations due to sensory impairments or when the environment has few quality stimuli.
Sensory impairment: Any type of difficulty that an individual has with one of their five senses or sensory function.
Sensory overload: A condition that occurs when an individual receives too many stimuli or cannot selectively filter meaningful stimuli.
Somatosensation: Sensory receptors that respond to specific stimuli such as pain, pressure, temperature, and vibration; includes vestibular sensation and proprioception.
Tinnitus: Hearing ringing in the ears.
Vestibular sensation: A sense of spatial orientation and balance.
Learning Objectives
- Assess the patient for objective and subjective manifestations of impaired oxygenation
- Distinguish normal and abnormal assessment data
- Adapt care based on oxygenation assessment data
- Interpret diagnostic tests and lab values indicative of a disturbance in oxygenation
- Identify evidence-based practices
Sufficient oxygenation is vital to maintain life. When prioritizing nursing interventions, we often refer to using the “ABCs,” an acronym used to signify the importance of maintaining a patient’s airway, breathing, and circulation. Several body systems work collaboratively during the oxygenation process to take in oxygen from the air, carry it through the bloodstream, and adequately oxygenate tissues. It is important that all parts of the system work together to ensure that oxygen is delivered appropriately to tissues within each system. Any alteration in these systems can have catastrophic implications on a patient’s health. First, the airway must be open and clear. The chest and lungs must mechanically move air in and out of the lungs. The bronchial airways must be open so that air can reach the alveoli, where the exchange of oxygen and carbon dioxide occurs. The heart must effectively pump oxygenated blood from the lungs and through the systemic arteries. There must be adequate amounts of hemoglobin in the blood to sufficiently carry the oxygen molecules to the tissues. However, several medical conditions such as asthma, chronic obstructive pulmonary disease (COPD), pneumonia, heart disease, and anemia can impair the body’s ability to effectively complete this oxygenation process.[1] This chapter will review these basic concepts related to oxygenation and apply the nursing process to patients who are experiencing alterations in oxygenation.
Learning Objectives
- Assess the patient for objective and subjective manifestations of impaired oxygenation
- Distinguish normal and abnormal assessment data
- Adapt care based on oxygenation assessment data
- Interpret diagnostic tests and lab values indicative of a disturbance in oxygenation
- Identify evidence-based practices
Sufficient oxygenation is vital to maintain life. When prioritizing nursing interventions, we often refer to using the “ABCs,” an acronym used to signify the importance of maintaining a patient’s airway, breathing, and circulation. Several body systems work collaboratively during the oxygenation process to take in oxygen from the air, carry it through the bloodstream, and adequately oxygenate tissues. It is important that all parts of the system work together to ensure that oxygen is delivered appropriately to tissues within each system. Any alteration in these systems can have catastrophic implications on a patient’s health. First, the airway must be open and clear. The chest and lungs must mechanically move air in and out of the lungs. The bronchial airways must be open so that air can reach the alveoli, where the exchange of oxygen and carbon dioxide occurs. The heart must effectively pump oxygenated blood from the lungs and through the systemic arteries. There must be adequate amounts of hemoglobin in the blood to sufficiently carry the oxygen molecules to the tissues. However, several medical conditions such as asthma, chronic obstructive pulmonary disease (COPD), pneumonia, heart disease, and anemia can impair the body’s ability to effectively complete this oxygenation process.[2] This chapter will review these basic concepts related to oxygenation and apply the nursing process to patients who are experiencing alterations in oxygenation.

